
ERRORS IN PATHOLOGY REPORTS
A wrong pathology report can be one of the following categories :
1.It is ' thought ' to be wrong ( " The doctor ' thinks ' that is a wrong report ! " tells us the relative.) though the pathologist had taken all due care, before he signed the report, and
2.A real wrong report.
In my experience, the first category mistakes are many in number in actual practice. When a test is actually done by the pathologist, with use of good standard and usually by the best available method, it is disregarded by the clinician by saying, " I do not think that his glucose is this much ", or " his haemoglobin is this much " from his past clinical experience. This happens almost every day with glucose estimation. A pathologist must be definitely seeing more diabetic patients every day, with their glucose levels. I can say, that there is no correlation in most patients. We have seen many patients with glucose levels around 350 - 400 mg /dl with absolutely no signs and symptoms. In many patients, this is the first detected raised glucose level. We always take due precautions by repeating the tests, -- and a possibility of wrong labeling the sample bottles is almost nil in a private laboratory - such reports are just discarded by the referring doctor by saying, " I do not think this report is correct. A patient should be in coma with such a level. What happens, some times, the bottles are interchanged (an effect of knowledge gained from Hindi movies or TV serials!), and hence such a report.". " I will send the blood to another laboratory tomorrow and repeat the test.". Next day , the patient, already alarmed, gets good morning exercise, takes low calorie diet, avoiding sweets.. and also takes his forgotten medicine for diabetes, if he already had!. Then all this is well reflected in his next reading. Then comes a happy remark, " Didn't I tell you, it was a wrong report ? "
I just wish to discard this group from my discussion, as this, thus, is more ' thought ' as a mistake, than is actually true !. As the only solution is improvement in thought process of the clinician, this is beyond scope of a pathology laboratory.
THE REALLY WRONG REPORT: These also are common, but one should know the following fact. A pathology report is an end product of a long chain of actions. Any mistake at any step will be a reason for wrong report. The steps can be summarized as :
I. Patient preparation :
a. time of the day.
b. Fasting / non
fasting / PP
II Specimen collection :
a. venepuncture technique
b. Proper bulb selection
-proper anticoagulants
-proper proportion.
c. Correct labeling.
III Specimen handling:
a.Transport
b.Processing
c. Storage.
IV Analysis :
a.Method Precision ( Coefficient of Variation )
b.Method accuracy ( Calibration )
c. Quality of Reagents.
V Reporting :
a.Calculations
b.Transcription
c.Typing
d. Proper
distribution : correct report goes to proper patient.
In most cases of out - of - lab collections, steps I, II and III are totally neglected. A laboratory is responsible in these cases for steps IV and V only. If the blood sample is collected in side the laboratory, then steps II, IV and V come in play. But for step I only the patient is responsible.
This is how all the steps play their part :
I. Patient Preparation :
a. Time of day : Many blood constituents, especially the haematological, show physiological variations during the day ( ' Diurnal variations ' ).
b. Fasting / Non -fasting / PP samples : Only a few patients follow our instructions about such preparation. Many consume tea /coffee, biscuits, prasad after pooja , etc, but tell us that they are fasting ! In spite of our detailed instructions, they do not follow the PP sample instructions. Another point makes a significant difference in blood glucose levels. For fasting glucose estimation, they come to lab by rickshaw. Next time, they walk up to the lab, which alters blood glucose level.
II. Specimen collection :
a. Venepuncture technique: i. Longer application of tourniquet produces haemoconcentration, raising Hb and all other counts. ii.Wet syringes produce haemolysis, changing many biochemical values.
b. Selection of proper collection bulbs: It is an important factor. Bulb for glucose must contain sodium fluoride, so that glycolysis, which starts after about 30 mins after collection, is prevented. But the same chemical being toxic to enzymes, the enzyme dependant tests, like urea, creatinine, serum enzymes, reduces the values markedly and hence should not be used for such tests. ( Many times, blood samples are collected in one bulb only for CBC, glucose, urea, creatinine and cholesterol ! ). Also the preparation of the anticoagulants should be proper. Even preparation of such bulbs matters : Adding 1 - 2 granules of anticoagulants powder produces macrocoagulation if not properly swirled immediately. Bulbs prepared by adding dissolved anticoagulant in proper portion and then drying is the best method. Citrate bulb for prothrombin time contains citrate solution just necessary and sufficient for 2 ml blood. Smaller or larger quantity of blood by itself alters prothrombin time significantly.
c. Correct labeling of samples : Incorrect labeling is more likely to occur outside the labs.In the wards, blood is usually collected by nursing staff. The collection of various specimens becomes just a small part of their work. The staff members really are many a times pressed by large amount of other nursing work, like taking TPR, BP, attending the medical rounds, giving injections and tablets as prescribed and making notes of all of these. This pressure is increased in emergencies, operation, post- op care, etc. So the mistakes are more possible in such cases. On the other hand, in lab, one person is engaged for only collection of the specimen. It is customary to collect all specimens till a specific time, so that only work during these hours is collection of blood / other samples and their arranging in proper groups. As a routine, always the blood collection bottle is labeled before taking out the blood. Hence, the chance of wrong collection or identification in lab is almost nil.
III.Specimen handling : Invariably, the samples from a hospital are transported in a plastic cover ( of an I V set ) after sealing the specimen bottles by adhesive tapes. In most cases, blood leaks through the bulbs as they topple in various positions. What a variety of changes in constitution such a leak makes !
Fig 1:  The bulb leaks while in
erect position. (by say jerks because of irregular road surface) : The
plasma comes out leaving cell concentrate in the bottle.
The bulb leaks while in
erect position. (by say jerks because of irregular road surface) : The
plasma comes out leaving cell concentrate in the bottle.
Fig 2.  If the bulb topples down and starts leaking immediately, whole blood comes out, which may not change the proportions. If, however, the blood starts leaking after some times, as RBCs settle, more and more packed cells leak out, leaving the diluted blood in the bulb.
If the bulb topples down and starts leaking immediately, whole blood comes out, which may not change the proportions. If, however, the blood starts leaking after some times, as RBCs settle, more and more packed cells leak out, leaving the diluted blood in the bulb.
Fig 3. 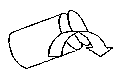 If the bulb tilts, and then leaks, then depending upon time lapse ( so that more and more RBCs settle down, and more and more plasma comes at the top ), the blood leaks, and the constituents change.
If the bulb tilts, and then leaks, then depending upon time lapse ( so that more and more RBCs settle down, and more and more plasma comes at the top ), the blood leaks, and the constituents change.
Thus blood which reaches our labs may be totally different in constituents than when it was collected. This can be very easily prevented by sending the samples in a box in an erect position ( which is rarely done ! )
The delay in sending to lab ( some times for many hours ) and storage in improper condition ( like in sunshine in a window, near a heating instrument, etc. ) also play their role in changing both the biochemical and haematological constituents.
IV. Factors dependent on analysis. Very commonly, a test done on the same sample in two different laboratories gives two different results. It may not be a real mistake. Please note the following before blaming any one report.
If a test is repeated 20 times by the same technician, by the same set of instruments on the same sample, the results definitely vary. Variation up to a value of + / - 2 SD is taken as correct report any where in the world, including in the developed countries. And one of the 20 readings may normally go beyond + / - 2 SD levels. This is an accepted fact.
Standard deviation for glucose is accepted up to +/- 4.5 mg /dl. It means, if a glucose standard of 100 mg % is run 20 times in a test, the results may vary from 91 mg / dl to 109 mg / dl ( +/- 9 ), and one result may go beyond this range normally. Similarly, a plasma of 200 mg / dl may show readings from 182 to 218 mg / dl, and this is accepted as a correct value by those who know about Medical Statistics, Standard Deviation and Precision of a test. ( This fact also brings out the ' more correctness ' of a glucose value expressed in 2 decimals, like 182 . 26 mg / dl ! )
This value of + / - 2 SD is different for different biochemical tests, which is accepted as a correct value for those tests is given in a table below :
From ' Average relative standard deviation values found for various analyses, data from Ross J W and Fraser A M , Am J Clin Path, 68 ( Suppl 1 ) - 130, 1977 )
|
Constituent |
Conc. Level |
% SD |
Range |
|
|
|
|
|
|
Glucose |
70 mg % |
4.0 |
64.4 - 75.6 mg% |
|
|
160 |
3.1 |
150.1 - 169.9 |
|
|
220 |
3.2 |
206 - 234 |
|
Urea |
10 mg % |
4.9 |
9 - 11 |
|
|
50 |
3.6 |
46 - 54 |
|
|
80 |
4.6 |
72 - 87 |
|
Cholesterol |
120 mg % |
4.6 |
109 - 131 |
|
|
220 |
4.6 |
199 - 241 |
|
Bilirubin |
0 .7 mg% |
15 |
0 . 5 - 0 . 9 |
|
|
1. 0 |
13 |
0 . 7 - 1 . 3 |
|
|
1. 5 |
6.3 |
1 . 3 - 1 . 7 |
|
|
2. 0 |
5.0 |
1. .8 - 2. 2 |
|
|
6. 0 |
4.8 |
5 . 4 - 6 .6 |
|
Creatinine |
1. 0 mg% |
7.9 |
0. 8 - 1 . 2 |
|
|
1 5 |
6 .2 |
1 . 3 - 1 . 7 |
|
|
2 . 0 |
5. 0 |
1 . 8 - 2 . 2 |
|
|
6 . 0 |
3. 6 |
5 . 6 6 . 4 |
|
|
|
|
|
|
|
|
|
|
It means, in general a variation of this much amount is accepted as just a normal variation. Hence, this much of a difference is possible in the same laboratory. Translate this difference when this test is done in two different laboratories, which different reagents, by different methods and by two different persons.
For accuracy, we are totally dependent on all chemicals prepared by various companies. The quality of results greatly depends on manufacturing of these reagents, their packing, transport and their storage at various levels, upto the laboratory. ( In a separate article, I have compared marked variation in results of different glucose reagents, on one and the same sample ). All these factors are beyond control of a pathology laboratory. We can only stop use of poor reagents by experience, which we always do.
V.Reporting: Mistakes due to wrong calculations, faulty transcription, defective typing and improper distribution of the reports are almost totally because of negligence laboratory personnel. They are inversely proportional to the concentration of mind. More than normal work, less work, heated discussions with the patient / relatives / doctor / colleagues, etc. are the reasons. They should be frankly admitted by the laboratory personnel, and improvement in this subject can be tried.
The details given above are not to shed our responsibility for mistakes in pathology report, but just to give outline of whole procedure of preparation of any pathology report. One should understand that this is an end product of such a long chain, and hence only a pathologist who signs the report and types the report ( the only legible paper in this chain ! ) should not be held responsible for it. This article is written to help the pathologists to analyze their so called wrong reports and to conclude whether it was a really wrong report or a 'thought as wrong report !
Dr. Pramod Vaman Purohit
Consulting Pathologist
347, E , Opp Railway Station
Kolhapur, 416 001 ( Maharashtra )
E-mail: kpr_pathpuro@sancharnet.in